POSTERIOR, ANTERIOR … WHERE AND WHY IN THE EYE?
For reasons of tradition, physical accessibility and function, the eyeball is typically divided into two segments: the anterior (front) segment and the posterior (rear) segment. A simplified description is as follows.
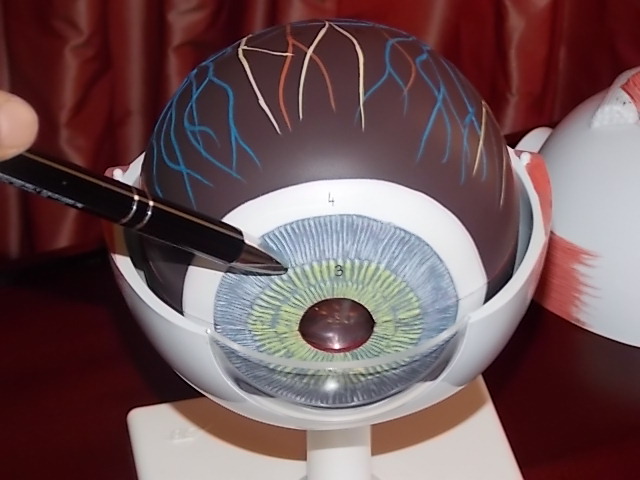
Viewed from the front, your eye is made up of the following structures, from front to back: the clear conjunctiva, then the clear – and sensitive – cornea, which bulge to form a small hollow towards the front of the eye (the anterior chamber), behind which is that familiar to us as the individual coloration of the eye (blue, green, brown eyes): the iris with the pupil in the centre: the black, movable aperture that lets light into the eye, behind which lies the eye’s circular, natural lens.
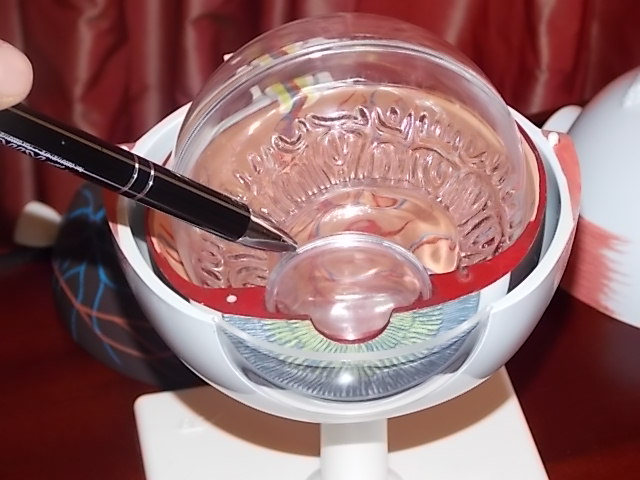
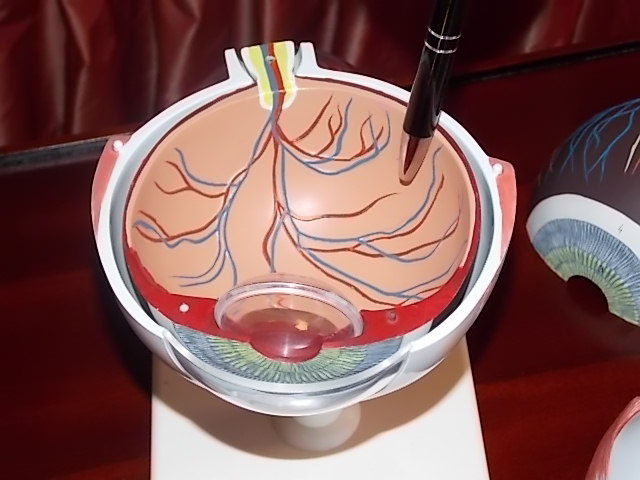
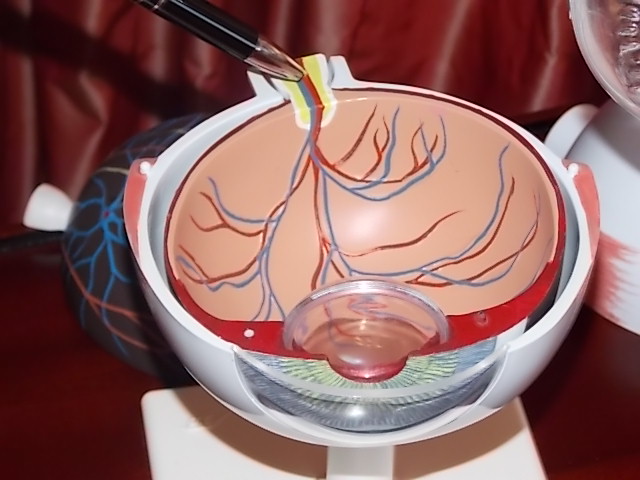
In medical terms, the back of the eye begins behind the lens. None of this can be seen simply by looking at the eye. Immediately behind the pupil and the lens is located the gelatinous mass that forms the bulk of the eye (the vitreous body, which is a large, removable transparent ball in the eye model) and, right at the end, in the last part of the eyeball, the retina, which covers the rear hemisphere of the eye like wallpaper, including the vessels of the retina visible to the ophthalmologist during an eye exam, with their typically reddish-orange light reflex. The macula is in fact just a special location on the retina with particular cellular characteristics and functionality. Located right at the back of the eye is the optic nerve, which bundles together all of the nerve fibres of the retina, exiting the eye at the rear to link up to the brain. Our brains identify and sort out the visual images that we see with our eyes.
Much simplified, we can say that the front of the eye regulates the incidence of light to ensure that an image can be formed at the back of the eye on the retina. Our vision is dependent on light being regulated to fall so that it hits the retina precisely – not too far in front and not too far behind. If the eye in the posterior segment is healthy but light incidence is less than ideal, “helper lenses” in glasses and contact lenses regulate the incidence of light to give us good vision: the lenses in these visual aids ensure that the light once again falls precisely on the retina. The general clouding-over of the eye’s natural lens (cataract) at the front of the eye, typically at an advanced age, can prevent light entering the eye: if it is replaced by an artificial lens (cataract operation), we can see clearly once again. In this case, the person’s actual vision is not yet affected: it is possible for the anterior segment to obstruct the entry of light or fail to focus it properly.
OPERATIONS IN THE POSTERIOR SEGMENT OF THE EYE REQUIRE MASTERY OF THE OPHTHALMIC ART.
At the back of the eye, the retina and macula are decisive in enabling us to see anything at all – to actually form a visual image. Located at the back, the eye’s retina and macula regulate the quality of the image, whether we see colour or a distorted image, etc. The macula, the place at which vision is the sharpest, is instrumental for the quality of our high-resolution vision – such as is required for reading. If deposition, new vessel formation or occlusion, bleeding or a tear occurs here in the retina and – above all – the macula, severe visual impairment often results. The operations and techniques used for the posterior segment of the eye are necessary in order to treat disorders so as to maintain either visual acuity or eyesight itself. The demands and responsibilities placed on the surgeon for operations in the posterior segment are quite different to those in the anterior segment. Experts in the posterior segment are correspondingly hard to find among practising ophthalmic surgeons.
COMBINED OPERATIONS
Our hospital routinely handles operations both in the anterior segment and in the posterior segment. Our combined operation service – namely carrying out surgical interventions to the anterior and posterior segments of the patient’s eye in a single operation – is a speciality of our Centre available only to a very few qualified ophthalmic surgeons. With the exception of administering medication to the vitreous body, most practising eye surgeons are not trained for surgery involving the posterior segment of the eye. See also: Our 360° eye expertise makes the difference.
OPERATIONS WE PERFORM IN THE POSTERIOR SEGMENT:
- Intravitreal injections (administration of medicine, injections into the vitreous body) for patients with macular degeneration and other macular disorders (Lucentis, Macugen, Avastin, Triamcinolon, Eyelea, etc.)
- Scleral buckling surgery for retinal detachment and retinal tears
- Vitrectomy with and without endotamponade (gas, oil, heavy liquids) for simple and complicated retinal detachments (vitreous body/retinal operations)
- Epiretinal and subretinal membrane surgery (removal of membranes/bleeding on and underneath the retina)
- Macular translocation (rotation of the entire retina)
- Intraoperative laser treatments and cold treatments for the retina in relation to vitrectomy
- Combined operations: vitrectomy and cataract surgery
OPERATIONS WE PERFORM IN THE ANTERIOR SEGMENT:
Supplementing our specialist work in the posterior segment, we also offer our patients the latest innovations and surgical techniques for the anterior segment.
- Cataract surgery. Our Centre not only carries out the standard cataract operation with many options for anaesthesia, but also offers you the opportunity to replace your natural lens with a lens that corrects your vision. By selecting this option in addition to cataract surgery, your new lens will also replace your glasses. We are one of only ten centres in Germany that have started supplementing their ranges of single vision, multifocal and cylindrical lenses (toric lenses) with the very latest innovation – the LAL (Light Adjustable Lens). Following your operation, a straightforward process using UV light (and with no side effects) is used to calibrate the LAL in your eye precisely to your visual needs, ensuring that you no longer need glasses to focus on faraway objects.
- ICL – the intraocular contact lens that replaces your glasses
- Penetrating/lamellar keratoplasty (corneal transplantation)
- Reconstructive anterior segment surgery following injury
- New innovation: Specialised lens implants for advanced macular degeneration ‒ In cases where incident light normally falls onto damaged parts of the retina no longer available to the patient for vision, an additional lens system (VIP-IOL) is used to redirect this light onto intact portions of the retina.
- Operations for lowering intraocular pressure in glaucoma, using a wide range of surgical techniques
- Wir führen bereits seit 2012 augendrucksenkende Operationen mittels ECP Lasertechnik durch
- In 2012, our Centre started offering operations for lowering intraocular pressure with ECP laser technology viacross-linking. Cross-Linking is a new method for treating keratoconus – an often progressive change in the cornea that creates problems with vision.
- Operations commonly combined, such as cataract surgery and ECP (lowering intraocular pressure in glaucoma)
LASER-ASSISTED SURGERY
- Laser coagulation for diabetic or other changes to the vessels of the retina or retinal tears
- YAG laser capsulotomy for secondary cataracts following cataract operations
- Laser trabeculoplasty for glaucoma
- Laser iridotomy for glaucoma
- Laser polishing of an artificial lens following inflammation
- PDT (photodynamic treatment) for age-related macular degeneration
SAY GOODBYE TO YOUR GLASSES – LENS IMPLANT OPTIONS FOR SAFE, LONG-TERM GOOD VISION
Many patients would love to be free of the need to wear glasses. For an ophthalmologist’s perspective, an eye that requires glasses or contact lenses to correct for 100% visual acuity is still a healthy eye. Any surgical intervention in a healthy eye must therefore be conducted with extreme care: even if the risks are today very low, they are still present. If you would like to be able to stop wearing glases, we can offer you what is in our opinion the best technique currently available, namely an intraocular lens implant.These work like contact lenses, but instead of being placed outside – on the conjunctiva and cornea – are placed inside the eye (intraocular) in front of the natural lens.These lenses have the major advantage of being removable at any time in the future, thereby restoring the original natural condition of the eye.Unlike laser-assisted techniques (such as LASIK), intraocular contact lenses (ICLs) are therefore a sophisticated and fully reversible procedure that leaves the healthy eye intact. ICLs can be adjusted to the patient’s personal needs – refractory changes, development of a cataract or (at an advanced age) other eye disorders – and to correct visual deficiencies. We recommend ICLs to all patients seeking a safe, reversible and long-term alternative to wearing glasses.In our opinion, laser-assisted correction of defective vision (LASIK) is not to be recommended for a great many reasons, the most important of which being the irreversible changes it introduces into the cornea. While it is a technically simply procedure, it is not a technique that is offered by our Centre.
Please contact our Centre for further advice. More information, including announcements of patient information events, is available from our website.